I. ANATOMICAL FEATURES
A thorough understanding of orbital anatomy is essential in evaluation of orbital neoplasms.
The primary location of a lesion can help guide the differential diagnostic and meticulous descriptions of lesion location,
involved structures and extent can enable proper treatment planning.
The bony orbit comprises four walls,
four rims and the apex.
The medial wall is represented predominantly by the lamina papyracea,
a thin portion of the ethmoid bone.
Anterior to the lamina papyracea is the lacrimal bone (containing the nasolacrimal duct) and the frontal process of the maxillary bone.
Posterior to the lamina papyracea is the lesser wing of the sphenoid.
The lateral wall is the thickest wall of the orbit and is formed by the greater wing of the sphenoid posteriorly and the frontal process of the zygomatic bone anteriorly,
which meet at the zygomaticsphenoid suture.
The superior wall or the roof is formed by the orbital plate of the frontal bone and posteriorly by a part of the lesser wing of the sphenoid near the apex.
The superior orbital fissure is the space between the greater and lesser wings of the sphenoid bone.
The supraorbital foramen lies lateral to the frontal sinus and contains the supraorbital nerve (the first division of the trigeminal nerve or V1).
The inferior wall or the floor is formed by the orbital surface of the maxillary bone,
the orbital surface of the zygomatic bone and the orbital process of the palatine bone.
It is separated from the lateral wall by the inferior orbital fissure.
The infraorbital foramen contains the infraorbital artery and vein and the infraorbital nerve,
branch of the maxillary nerve,
is located approximately in the centre of the inferior wall.
The nasolacrimal foramen is located medially,
near the orbital margin.
Both the supraorbital and infraorbital foramina are important as potential pathways for cancer and infections of the orbit to spread into the brain or other deep facial structures.
The apex is where all four walls of the orbit converge.
The optic canal,
containing the optic nerve and the ophthalmic artery,
lies between the two roots of the lesser wing of the sphenoid.
The four orbital rims are formed by the frontal bone,
the zygomatic and maxillary bones.
The globe is surrounded by three major tissue layers: the outer layer is the white sclera and anteriorly the cornea,
the middle layer is the uveal tract (consisting of the choroid,
iris and ciliary body) and the internal layer is the retina.
The lens and iris divide the globe cavity into an anterior chamber filled with aqueous humor,
and a posterior chamber filled with vitreous.
The optic nerve is about 5 cm long and is divided into four segments: intra-ocular,
intra-orbital,
intra-canalicular and intracranial.
The subarachnoid space between the dura and pia covering the optic nerve is continuous with that of the suprasellar cistern.
There are six extra-ocular muscles surrounding the globe: four rectus muscles and two oblique muscles.
The rectus muscles have a common origin,
the annulus of Zinn or the annular tendon (fibrous ring that encircles the optic nerve at its entrance in the apex) and insert into the sclera of the globe.
The superior oblique muscle originates from the lesser wing of the sphenoid,
hooks around the trochlea (posterior to the superior orbital rim) and the trochlear tendon inserts into the sclera beneath the tendon of the superior rectus muscle.
The inferior oblique muscle originates from the anteromedial aspect of the orbital floor near the lacrimal sac and inserts into the sclera after passing below the inferior rectus tendon.
The lateral rectus is innervated by the abducens nerve,
the superior oblique muscle by the trochlear nerve and all other muscles by the oculomotor nerve.
The levator palpebrae superiorus muscle,
innervated by sympathetic fibres,
originates from the lesser wing of the sphenoid and annulus of Zinn,
is located above and parallel to the superior rectus muscle and it inserts into the superior lid retractor system.
The superior rectus and levator palpebrae superiorus muscles are difficult to distinguish by imaging methods,
and therefore considered as a complex.
The lacrimal gland belongs to the extraconal space of the orbit anteriorly,
located superolateraly.
It has 2 component: an orbital part in the lacrimal fossa of the orbit on the lateral margin of the levator palpabrae superioris muscle extending into the orbital septum and a palpebral part.
Its structure is particular,
being composed of both epithelial and lymphoid tissue.
II. IMAGING
For the purpose of imaging interpretation and differential diagnosis,
it is usual practice when interpreting CT and MRI findings to assign a lesion to a certain compartment within the orbit: the globe,
the intraconal,
conal and extraconal compartments.
The intraconal compartment contains orbital fat,
the ophthalmic artery,
cranial nerves II and III as well as the optic nerve-shead complex,
containing the optic nerve,
the central retinal artery and vein and the surrounding sheath of meninges extending from the cerebral meninges.
The conal space contains the extraocular muscles,
the interconnecting fascia and cranial nerve VI.
The extraconal space contains the lacrimal gland and sac,
the superior ophthalmic vein and orbital fat.
When a disease is multicompartmental,
it is discussed in the section of the compartment where it arises or is present most frequently.
A. TUMOURS OF THE GLOBE
RETINOBLASTOMA
Retinoblastoma is the most common tumour of the globe in children,
affecting children less than 3 years old that with leukokoria.
The majority are unilateral unifocal,
but around 25 % are bilateral or unilateral multifocal.
Retinoblastoma is highly malignant and may spread haematogenously,
via lymphatics,
or along the optic nerve to the intracranial compartment and metastasize in the subarachnoid space.
Imaging is crucial for timely management and survival of patients with retinoblastoma.
It is imperative to perform cross-sectional imaging and not just rely on ophthalmoscopy,
in order to exclude other retrobulbar tumours with globe invasion and to asess optic nerve invasion and intracranial metastases.
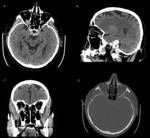
CT is the imaging method of choice for children with leukokoria because it is sensitive to calcifications (clumped or punctate,
in 95 % of cases).
A mass in the posterior part of the globe extending into the vitreous,
with calcifications and minimal enhancement is suggestive for retinoblastoma.
Absence of calcification means this diagnosis is unlikely
In advanced cases,
the tumour may fill the globe.
UVEAL MELANOMA
Uveal melanoma is the most common primary intra-ocular malignancy in adults.
The majority are unilaterall.
Patients present with decreased visual acuity,
retinal detachment or ocular pain.
It is highy invasive and can metastasize to the liver and lung.
Recurrence is common once extraocular spread develops.
Diagnosis usually requires only ophthalmoscopy and ultrasound.
CT and MRI are not part of the routine workup except when proper ophthalmoscopy is not possible.
CT and MRI show a soft tissue mass centred on the outer layers of the globe that bulges into the vitreous.
On CT it is hyperdense and enhances moderately.
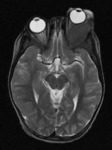
On MRI,
it is hyperintense on T1WI and hypointense on T2WI due to the presence of paramagnetic melanin with or without haemorrhage (fig.
3).
Amelanotic melanomas are hypointense on T1WI and hyperintense on T2WI,
like other tumours.
Both types of melanomas enhance.
MRI is better than CT for adequate differential diagnosis with choroidal haemangiomas and choroidal detachments and for better assessement of episcleral invasion.
Very seldom,
the majority of the globe may be involved.
OCULAR METASTASES
Only around half of the patients with ocular metastases have a known primary tumour,
usually from a malignancy in the lung,
breast or the gastrointestinal tract.
Ocular metastases occur mostly to the uveal tract.
They are seen on CT as small multiple areas of hyperdense thickening,
occasionally with subretinal fluid.
B. TUMORS OF THE CONAL COMPARTIMENT
PSEUDOTUMOUR
Pseudotumour is an inflammatory disease with rapid onset that presents in middle aged patients,
usually with unilateral painful ophthalmoplegia,
proptosis and chemosis.
The acute form has a proper response to steroids,
unlike the chronic form which requires chemotherapy or radiotherapy.
The ethology is probably autoimmune,
in 10 % of cases it accompanies other systemic autoimmune condition.
The changes seen on cross-sectional imaging may be found in any component of the orbit: the retrobulbar fat,
extra-ocular muscles,
optic nerve,
the uveal-scleral area or the lacrimal gland.
Two patterns may be recognized: the tumefactive type with diffuse involvement of conal or intraconal structures,
or the myositic type involving ususually a single extra-ocular muscle and its tendinous insertion.
Pseudotumours enhance after contrast administration.
On,
CT it can be seen as a subtle hyperdensity of intra-orbital fat. On MRI it is hypointense to fat on T2WI,
whereas true tumours are hyperintense to fat on T2WI.
RHABDOMYOSARCOMA
Rhabdomyosarcoma is one of the more common primary malignant tumours of the orbit in children aged 2–5.
It is highly malignant and presents with rapidly progressive exophthalmos.
It originates from the extra-ocular muscles,
the nasopharynx,
or the paranasal sinuses.
It is usually located in the superomedial orbit and may produce bone destruction.
On CT,
these bulky aggressive-looking masses are isodense or slightly hyperdense,
and show uniform enhancement with bone destruction in 40 % of cases and frequent ocular distortion.
On MRI they are of intermediate signal intensity on both T1 and T2 sequences.
C. TUMORS OF THE INTRACONAL COMPARTIMENT
LYMPHOMA
Orbital lymphoma presents in middle age with painless swelling progressing to proptosis,
affecting any structure in the orbit.
Orbital lymphoma is of the B-cell variety whereas Hodgkins disease of the orbit is rare.
There is a wide range of radiological findings in orbital lymphoma,
wether it is a well-defined hyperdense enhancing mass on CT,
or it produces diffuse infiltration leading to destruction of the orbital architecture.
It however moulds to the contour of the orbit without bone destruction (fig 5),
unless very aggressive.
The combination of PET/CT may be useful if lymphoma is suspected.
On MRI lymphoma have a non-specific appearance.
Differentiation of orbital lymphoma from pseudotumor may be challenging at imaging.
Findings like infiltration or thickening of ocular muscles favor a diagnosis of pseudotumor.
Studies suggest that pseudotumors are more commonly isointense relative to orbital fat on T2WI and that lymphomas can be differentiated from pseudotumor on the basis of apparent diffusion coefficient values.
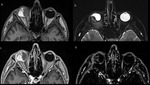
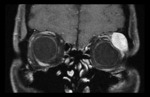
CAVERNOUS HAEMANGIOMA
Cavernous haemangioma is the most frequent benign orbital tumour that occurs in adults aged 20–40 and more commonly to men. Patients present with proptosis,
but with unaffected vision.
When the tumour is located in the region of the apex,
optic nerve compression may occur.
Extraconal location is also possible (fig.
1).
They contain large vascular spaces with a dense pseudocapsule,
but without recognizable arterial feeding vessel or draining vein,
and may have phleboliths and surrounding haemosiderin- ferritin deposits,
though intralesional haemorrhage is rare.
CT and MRI usually show rounded or oval mass with sharp contours that spares the orbital apex (fig.
1).
Bony deformity due to erosion may happen,
but no bone destruction.
These lesions are hyperdense and enhancing on CT scans.
MRI helps asses the optic nerve as well as extra-ocular muscles.
They are isointense or hypointense on T1WI and hyperintense on T2WI,
and enhance.
Different enhancement patterns can help differentiating between haemangiomas and other tumours.
CAPILLARY HAEMANGIOMA
This lesion is found in children less than 1 year old,
who present with proptosis.
It represents a proliferation of endothelial cells with numerous capillaries that regresses spontaneously in later years.
It may belong either to the intraconal or extraconal compartments.
Both CT and MRI show an enhancing and not very sharply demarcated mass.
MRI is the imaging method of choice to demonstrate punctate hypointense flow voids corresponding to dilated vessels.
Phleboliths are rarely seen.
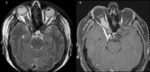
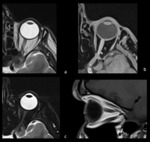
OPTIC NERVE MENINGIOMA
Optic nerve meningiomas usually affect middle-aged women and children with type 2 neurofibromatosis.
They develop from the arachnoid layer of the meninges as a tubular thickening and surround the optic nerve without infiltrating it (fig.
4),
but may also arise from the periorbital (periosteum of the orbita) which continues the dura mater.
In neurofibromatosis 1 or 2 they can be bilateral.
Intracranial spread can happen,
but only up to the prechiasmatic optic nerve sheath.
Remodelling of the optic canal and hyperostosis can be present.
On CT,
the lesions are hyperdense and enhance strongly,
thus producing a “tram track” sign on axial images or a “doughnut sign” on coronal images.
They may be calcified in less than 50% of cases.
On MRI,
the appearance is hypointense on T1WI and hyperintense on T2WI with strong enhancement,
thus T1 fat-suppressed post-contrast images are very useful in detecting early meningiomas.
OPTIC NERVE GLIOMA
Optic nerve gliomas are slow-growing low-grade pilocytic astrocytomas,
the majority of cases occurring in children less than 10 years old,
causing deteriorating vision and minimal proptosis.
Bilateral tumours can happen and are pathognomonic of neurofibromatosis type 1.
The lesion is represented by a thickening of the optic nerve/sheath complex that can be tubular,
fusiform or excrescent.
Unlike optic nerve meningiomas,
they cannot be separated from the optic nerve itself.
Enhancement occurs in 50% of cases.
Intralesional cysts may pe present but calcifications are rare.
MRI is useful to detect asses the optic pathways although an optic nerve glioma does not itself tend to spread from the optic nerve to the intracranial compartment.
D. TUMORS OF THE EXTRACONAL COMPARTIMENT
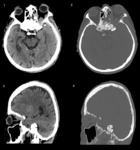
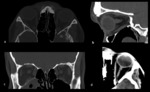
RETROBULBAR METASTASES
Most retrobulbar metastases are extraconal in location but can extend to the intraconal.
They originate mostly from the greater wing of the sphenoid,
resulting in bone destruction (fig.
2).
In children,
neuroblastoma or Ewing's sarcoma produce extraconal masses related to the posterior lateral wall of the orbit.
In adults,
an infiltrative retrobulbar mass is most clikely to be a breast carcinoma metastasis.
PLEOMORPHIC ADENOMA
Pleomorphic adenoma is the most common benign lesion of the lacrimal gland.
It is a slow-growing tumor that occurs in patients 40-50 yeards old; it often displaces the globe downward and causes proptosis.
At CT and MR imaging,
the lesion appears as a sharp delineated,
homogeneously enhancing mass in the superotemporal orbit (fig.
6).
Large lesions may become heterogene due to cystic degeneration,
hemorrhage,
serous or mucous collections,
or necrosis.
Because of its slow growth,
it may remodel the bone.
Bone erosion is rare and highly suggestive of malignancy.
Lesions are typically hypointense on T1WI and hyperintense on T2WI.
Pleomorphic adenomas should be excised altogether without biopsy,
since partial excision or rupture of the tumor may lead to recurrence or malignant transformation.
ADENOID CYSTIC CARCINOMA
Adenoid cystic carcinoma is the most frequent malignancy of the lacrimal gland.
It is very infiltrative with fast perineural spread.
Complete resection is difficult and the prognosis is poor.
At imaging,
early lesions are hard to differentiate from pleomorphic adenoma since irregular margins and distortion of orbital contents is seen only in advanced stages.
Bone erosion and calcifications are often.